Histamine Intolerance Symptoms vs. Food Sensitivity Symptoms: How to Tell the Difference
- Dig Nutrition
- Feb 8
- 8 min read

Maya thought she was doing everything right!
She'd spent the last six months overhauling her diet: ditching processed foods, loading up on organic produce, fermenting her own sauerkraut, adding avocado to literally everything. Her Instagram feed was basically a shrine to "clean eating." She meal-prepped spinach salads, sipped bone broth, and even started taking a probiotic that cost more than her monthly Netflix subscription.
But instead of feeling like the glowing wellness goddess she'd envisioned, Maya felt like her body was actively rebelling against her!
The bloating was so bad she looked six months pregnant by dinner. The migraines came out of nowhere: pounding, relentless, immune to every painkiller she tried. And the rashes? They'd appear on her arms and chest like some kind of mystery hive situation, then disappear just as randomly. Her brain fog made her forget mid-sentence what she was even talking about.
"I don't get it," she told me during our first call, voice cracking with frustration. "I'm eating all the healthy foods. Why do I feel worse than when I was living off takeout?!"
In Maya's case, many of those "superfoods" she was loading up on: avocado, spinach, sauerkraut, bone broth: were sky-high in histamine, a compound her body couldn't properly clear!
Maya didn't have a food sensitivity. She had histamine intolerance (a type of food intolerance). And once we figured that out, everything changed.

What Keeps You Stuck
If you've ever Googled your symptoms at 2 a.m. (no judgment: we've all been there), you've probably noticed that food sensitivities and histamine intolerance sound eerily similar.
Bloating? Check.
Headaches? Yep. F
atigue, rashes, digestive mayhem?
All of the above.
So how the heck are you supposed to know which one you're dealing with?
The truth is, they're fundamentally different problems, even though they show up in similar ways. Understanding the difference is the key to figuring out what's actually going on in your body: and more importantly, what to try next to support your system.
Let's break it down!
What Food Sensitivities Actually Are
First: quick (but important!) vocab cleanup, because these terms get mashed together online and it makes everything 10x more confusing.
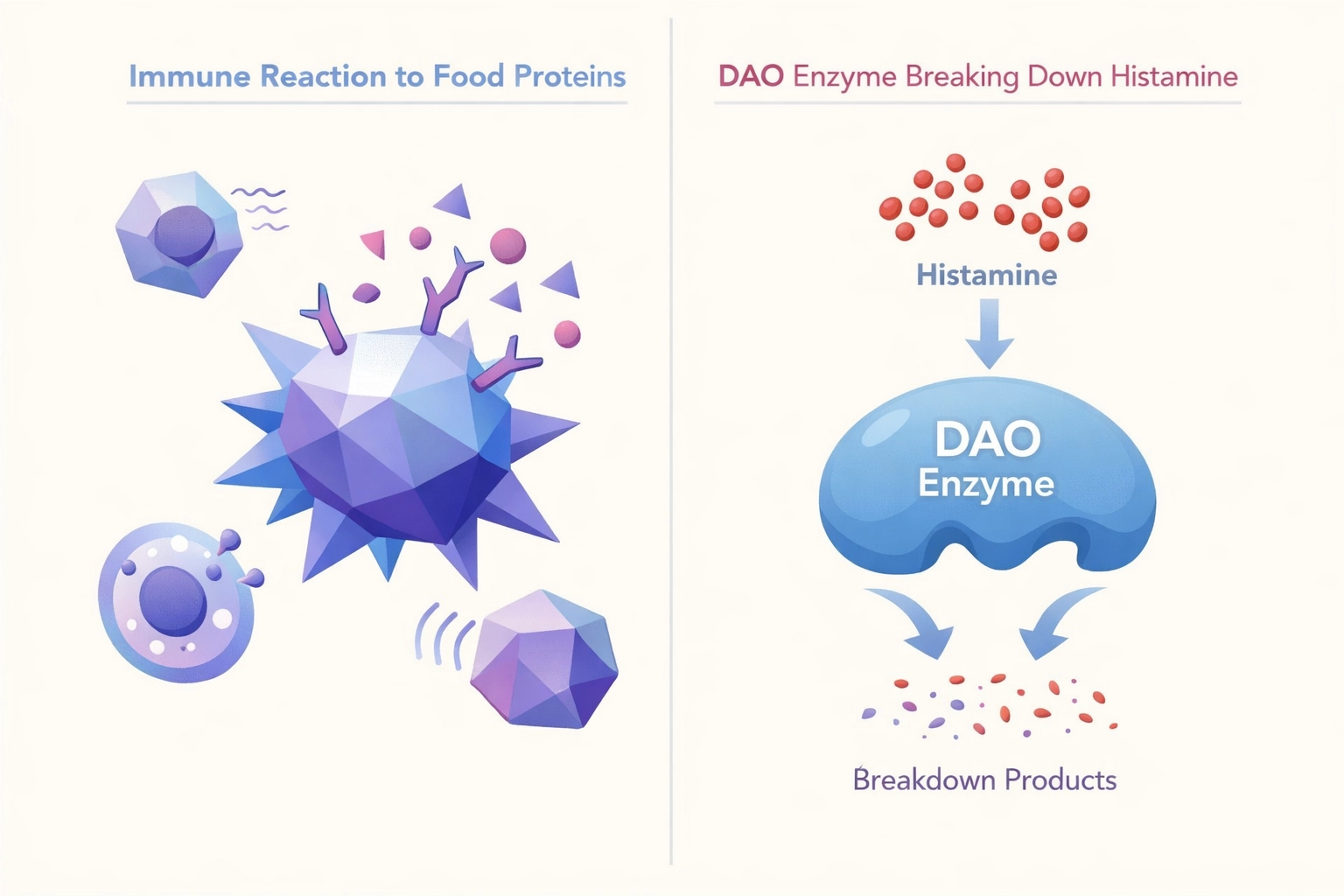
Food intolerance = a digestive/enzyme issue. Your body struggles to break something down (think lactose intolerance, or histamine intolerance when DAO is too low). Not fun, but also not your immune system “attacking” you.
Food sensitivity = an immune system issue. Your body flags certain proteins in food as a threat. Think of it like your body's security system mistakenly flagging a friendly visitor as a danger.
So in this post, when we say food sensitivity, we mean immune-driven reactions. And when we say food intolerance, we mean enzyme/digestion-driven reactions.
Common food sensitivity culprits include:
Gluten
Dairy (specifically casein and whey proteins)
Eggs
Soy
Corn
Nuts
When you eat a food you're sensitive to, your immune system launches a delayed response: usually showing up anywhere from a few hours to a couple of days later. That's why it's so hard to pinpoint which food is causing the problem. You ate the eggs on Tuesday, but the headache didn't hit until Thursday!
Classic food sensitivity symptoms include:
Bloating and abdominal discomfort
Diarrhea or constipation
Skin issues (eczema, rashes, acne)
Migraines or headaches
Brain fog and difficulty concentrating
Fatigue and low energy
Joint pain
Mood swings or anxiety
Food sensitivities are typically chronic: meaning if you keep eating the trigger food, the symptoms keep showing up (or never really go away). Your body can stay in a pattern of low-grade immune activation, which is exhausting for your system.
What Histamine Intolerance Actually Is
Histamine intolerance is a completely different beast. It's not an immune reaction: it's an enzyme problem.
Here's the deal: Histamine is a chemical compound that's naturally present in certain foods and produced by your own body. It plays important roles in your immune response, digestion, and nervous system regulation. Under normal circumstances, your body produces an enzyme called diamine oxidase (DAO) that breaks down histamine so it doesn't accumulate.
But when you don't produce enough DAO (or something is blocking it from working properly), histamine can build up in your system like a bathtub with a clogged drain. And when histamine levels rise too high, your body can start reacting in ways that feel disproportionate and uncomfortable.
Here's what makes histamine intolerance tricky: certain foods are naturally high in histamine or trigger your body to release more of it. So you could be eating the "healthiest" foods on the planet and still feel terrible if your body can't process the histamine load.
High-histamine foods include:
Fermented foods (sauerkraut, kimchi, kombucha, yogurt)
Aged cheeses
Cured and processed meats (salami, bacon, deli meat)
Leftover meat (histamine increases as food sits)
Alcohol (especially red wine and beer)
Bone broth
Spinach and other leafy greens
Avocados
Tomatoes
Eggplant
Citrus fruits
Strawberries
Vinegar
Crazy, right? I recommend many of these foods all the time because they can be incredibly supportive for the gut and overall health. They aren’t “bad” foods. In the right context, they’re powerful tools.
The issue isn’t the food itself. It’s the situation. When someone is dealing with a higher histamine load or struggling to break histamine down efficiently, even nutrient-dense, traditionally healing foods can backfire.
The encouraging part is that this is often workable. By supporting digestion, enzyme activity, and overall gut resilience, many people can gradually improve their tolerance and bring these foods back in without the flare-ups.

How to Tell the Difference: The Key Clues
So how do you know if you're dealing with a food sensitivity (immune reaction) or a food intolerance (enzyme/digestion issue like histamine intolerance)? Here are the telltale signs!
1. The Timing
Food sensitivities (immune): Symptoms can show up hours to days after eating the trigger food. The delay makes it hard to connect the dots.
Food intolerances (enzyme/digestion: like histamine intolerance): Symptoms often show up within minutes to a few hours after eating the problem food: but they can also build up over time if you're eating them consistently.
2. The Pattern
Food sensitivities (immune): Reactions are typically consistent. When you eat a true trigger food, symptoms tend to follow each time, even if the intensity varies. The challenge is that these reactions are often delayed by hours or even days, which can make it difficult to connect the dots.
Food intolerances (enzyme/digestion: like histamine intolerance): Reactions can be inconsistent and dose-dependent. You might tolerate a small amount of avocado one day but have a massive reaction after eating a giant bowl of guacamole the next. It's about your total histamine "bucket" overflowing.
3. The Symptom Spread
Food sensitivities (immune): Symptoms are usually digestive-focused or show up as chronic inflammation (skin, joints, energy).
Food intolerances (enzyme/digestion: like histamine intolerance): Symptoms are all over the map: multi-system dysregulation. Research shows that over 90% of people with histamine intolerance experience gastrointestinal symptoms, with bloating being the most common (affecting 92% of clients). But it doesn't stop there.
Common histamine intolerance symptoms include:
Digestive: Bloating (the big one), diarrhea, constipation, nausea, abdominal cramping
Skin: Hives, rashes, flushing, itching
Respiratory: Nasal congestion, runny nose, sneezing, asthma-like symptoms
Neurological: Migraines, dizziness, brain fog, anxiety, insomnia
Cardiovascular: Heart palpitations, low blood pressure, rapid heartbeat
Hormonal: Worsening symptoms around your period (histamine and estrogen are BFFs in the worst way)
If your symptoms feel like they're everywhere and nowhere all at once, histamine intolerance is worth investigating!
4. The Response to Intervention
Food sensitivities (immune): Removing trigger foods helps, but it can take weeks or even months to see full improvement because you're dealing with chronic inflammation.
Food intolerances (enzyme/digestion: like histamine intolerance): Many people notice symptoms may improve within 2-4 weeks of trying a low-histamine approach. The response can feel faster because you're reducing the immediate histamine load rather than waiting for longer-term immune patterns to settle.
5. The "Healthy Food Paradox"
This is the big one.
If you’re leaning into more fermented foods, bone broth, avocados, and spinach — the foods so often praised for gut and overall health — and you feel worse instead of better: and you feel worse, that's a massive red flag for histamine intolerance.
Food sensitivities (immune reactions) don't typically get triggered by these foods (unless you're sensitive to something specific in them). But if your body can't clear histamine (an enzyme/digestion intolerance issue)? Those "superfoods" become your kryptonite.
Why This Matters (And What to Do Next)
Here's why figuring this out is so important: the solutions are different.
If you have a food sensitivity (immune-driven), the focus is often on identifying and removing your trigger foods, supporting gut barrier function, and working to uncover root causes that may be driving reactivity (like dysbiosis and overall digestive stress).
If you have a food intolerance (enzyme/digestion-driven) like histamine intolerance, the focus is often on supporting DAO function in the gut lining, where this enzyme is primarily produced and active in the small intestine, reducing your overall histamine load, and working to uncover why your body may not be clearing histamine efficiently (common contributors can include dysbiosis, SIBO, hormone patterns, nutrient status, certain medications, or genetic factors).
You can’t fix one by only looking at the other.
The tricky part is that these patterns overlap. An immune-driven food sensitivity can increase inflammation in the gut. That inflammation can shift the microbial terrain. Certain microbes can then produce more histamine or interfere with how well you break it down. Now your “histamine bucket” is fuller than it should be.
So yes, they can influence each other.
But influence is not the same thing as identity. A histamine issue and an immune-driven food sensitivity aren’t identical problems, even if they interact. If we lump them together, we miss nuance. If we separate them too rigidly, we miss the bigger picture.
The goal isn’t to pick one label and defend it. It’s to understand your physiology well enough to see which pattern is primary right now, and how the layers may be stacking.
Maya's Happy Ending (And Yours)
Remember Maya? Once we pinpointed that histamine was likely a big piece of her puzzle everything shifted.
We swapped out the high-histamine foods for fresh, low-histamine alternatives. We supported her DAO function with targeted nutrients. And we worked to uncover the digestive imbalances that may have been contributing in the first place.
Within the first few weeks, the shift was noticeable. The bloating eased instead of building as the day went on. Migraines that used to derail her week became less frequent, then far less intense. Her skin started settling down rather than flaring at random. Energy came back in pockets at first, then stretched longer. The brain fog lifted enough for her to finish thoughts without losing them. She didn’t feel “fixed” overnight, but she could feel her system calming, step by step, back toward baseline.
"I can't believe I was unknowingly making things worse with 'healthy' foods," she laughed during a follow-up call. "But honestly? I'm just relieved to finally understand what my body was trying to tell me."
That's the power of working toward the root cause instead of playing whack-a-mole with symptoms!
Ready to Figure Out What's Really Going On?
If you're reading this and thinking, "Wait… this sounds like me," you're not alone. And you don't have to figure it out by yourself.
Book a free strategy session and we’ll talk through your symptoms, your food patterns, and your history—then share a few supportive next steps that may make sense for you. If functional testing feels appropriate, we can also explain options so you can make an informed choice (no guessing games required).
Educational disclaimer: This post is for educational purposes only and is not medical advice. DIG Nutrition does not diagnose, treat, cure, or prevent any disease. Always consult your licensed healthcare provider for medical guidance and diagnosis.
Because you deserve to feel good in your body. And the right foods should support you feeling amazing, not like you're falling apart!



Comments